The government needs to address the opioid crisis—and that takes money
It's not enough to restrict the supply of pills. We need long-term treatment for people who are addicted, and we need to pay for it.
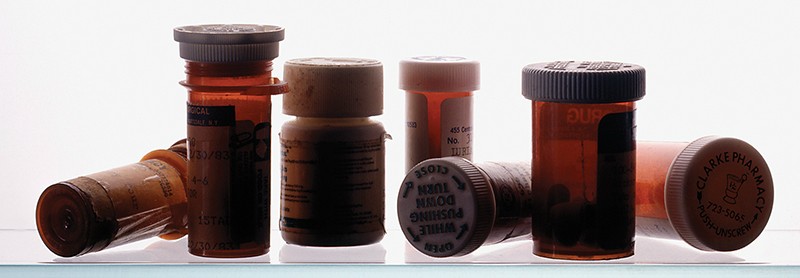
When a Vermont college student named Charlie (he does not want his full name used) hurt his knee playing hockey, his doctor prescribed opioid painkillers. Charlie’s story then followed a path typical for thousands of people: opioid use led to addiction, which led to the criminal use of heroin, which led to jail, which led to homelessness.
Charlie is one of the fortunate ones, however: he got treatment. Every day 91 opioid addicts in the United States die of an overdose. The opioid crisis killed more Americans in 2016 than were killed in the entire Vietnam War. Some 64,000 drug overdose deaths occurred that year, most of them opioid-related. The addiction problem has doubled in scope since 2010. Yet the country’s leaders remain slow to respond.
Read our latest issue or browse back issues.
The roots of the crisis are complex, but most experts agree that it started in doctors’ offices, where millions of patients like Charlie were prescribed opioid painkillers for short-term pain relief. Convinced by pharmaceutical companies that addiction to opiates was rare, doctors have dispensed these drugs freely. The amount of painkillers prescribed in 2016 was enough to provide them for every adult in the country.
Addressing the crisis involves two distinct and in some ways contradictory challenges. The first is helping the people already addicted. This cannot be done merely by cutting off the flow of painkillers, as some states have begun to do, as this is likely to send addicts in search of drugs that are even riskier, such as heroin. The second challenge is to prevent future addiction—which does entail cutting that flow of prescription pills.
In helping those addicted, the key step is to make treatment widely accessible and comprehensive, including medical therapy and social services. Vermont has shown the way on this front, using Medicaid funds to invest heavily in clinical treatment that uses methadone—itself an opioid—and other drugs to ease withdrawal and manage the addiction. Charlie credits this program with saving his life.
When it comes to preventing addiction, several states have sought to regulate opioids. Massachusetts was the first to limit the number of pills doctors can prescribe. Michigan places a seven-day limit on opioid prescriptions and provides an online database to prevent addicts from going from one doctor to another. In Colorado, Kaiser Permanente offers an eight-week course to help patients recognize the dangers of opioids and manage their pain through physical therapy, exercise, and meditation. As a result of that program, opioid use has dropped significantly.
Any comprehensive approach involving increased regulation and expanded treatment requires funding. Last October, President Trump declared the opioid crisis a national emergency but offered no additional money. Congress has allocated $1 billion over two years for drug treatment, but studies suggest that’s about a tenth of the money needed. Vermont officials estimate that it costs $16,600 to manage one person’s care. Compared to the cost of incarcerating someone for a year for illegal drug use—$31,300 a year—that’s a bargain. It’s also the only way to prevent more people from dying and more families and communities from being devastated.
FOLLOWING UP (Updated March 21): The two-year federal budget approved by Congress in early February added $6 billion in programs related to the opioid emergency. Some experts say that’s about half the money needed to provide treatment for those addicted.
A version of this article appears in the January 31 print edition under the title “In need of treatment.”






