Pfizer didn’t create its COVID vaccine alone
Yet it’s holding tight to its life-saving information—and its record-breaking profits.
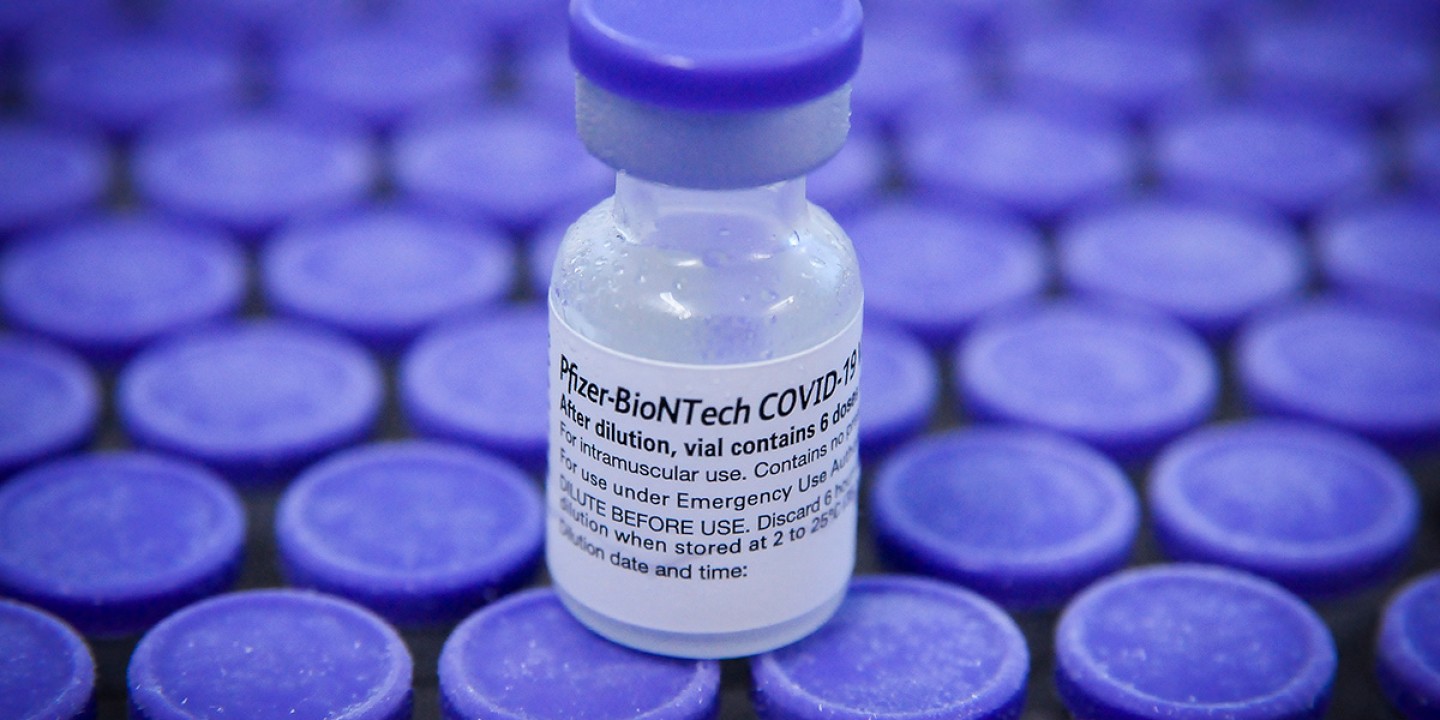
As of mid-February, 62 percent of the world’s population has received at least one dose of a COVID vaccine. The Access to COVID-19 Tools Accelerator, a global initiative backed by the World Health Organization, has delivered a half billion donated doses to poor countries. Another WHO-sponsored initiative has helped the South African company Afrigen formulate a new vaccine for Africa.
But these promising developments exist within a troubling context: the inequity that has plagued the vaccine rollout from the start. Rich countries have an 80 percent vaccination rate; in poor countries it’s 11 percent. Poor countries are still hurting for both vaccine doses and distribution networks—and the ACT Accelerator is hurting for cash, having received just 5 percent of the grants it expected from rich countries.
Read our latest issue or browse back issues.
As for Afrigen, Bloomberg reports that the team in South Africa spent precious resources piecing together a replica of the Moderna vaccine from bits of public information. That’s because the big pharmaceutical companies that own the existing intellectual property persist in refusing to share it. They continue to guard both their formulas and their logistical expertise as they focus on selling their own products.
They are stunningly profitable products. Pfizer recently disclosed that it made $81 billion last year—twice its 2020 profits, and nearly half of it from the vaccine alone. Pfizer anticipates breaking profit records again this year. From the start of the pandemic, the company has focused on maximizing profits. It has run a hard bargain on vaccine pricing. It has made mammoth deals both to vaccinate richer nations and to supply the doses they’ll donate elsewhere.
Debates about health-care funding often boil down to a question of priorities: Which matters more, the equity promoted by public financing or the innovation fostered by private investment? Last year, when the idea of a waiver for vaccine patents was gaining traction, Pfizer CEO Albert Bourla countered that companies need to retain the incentive to make risky investments during future pandemics. Vaccine inequity may be bad, the argument goes, but wouldn’t it be worse not to have the vaccines at all?
This is misleading. The vaccine was created not by Pfizer but by the smaller company BioNTech, through a project that relied on university research and public financing. A big company like Pfizer doesn’t innovate alone—if it innovates at all. Global Justice Now director Nick Dearden argues in the Guardian that such companies “behave more like hedge funds, buying up and controlling other firms and intellectual property, rather than traditional medical research companies.”
Respect for innovation shouldn’t mean fealty to the corporate profit motive. One lesson of this pandemic is that society must not leave something as crucial as a vaccine to the private sector’s whims. Instead we need governments to prioritize open sharing—via public funding, publicly available research, and nonexclusive manufacturing licenses—over the profits that can be wrung from intellectual property.
There’s no question that the profit motive can play a role in addressing global emergencies. But these two goals—profit and progress—can also come into conflict. When they do, which will prevail? The pharmaceutical industry and its government enablers have made their answer clear.
A version of this article appears in the print edition under the title “Whose vaccine?”





